Angermann CE, Assmus B, Anker SD, et al MEMS-HF Investigators. Shavelle DM, Desai AS, Abraham WT, et al CardioMEMS Post-Approval Study Investigators. Significant reductions in heart failure hospitalizations with the pulmonary artery pressure guided HF system: preliminary observations from the cardioMEMS post approval study. Costeffectiveness of implantable pulmonary artery pressure monitoring in chronic heart failure. Sandhu AT, Goldhaber-Fiebert JD, Owens DK, et al. Ambulatory hemodynamic monitoring reduces heart failure hospitalizations in “real-world” clinical practice. Hipertensión Pulmonar en las Cardiopatías Izquierdas 50ġ42. Sustained efficacy of pulmonary artery pressure to guide adjustment of chronic heart failure therapy: complete follow-up results from the CHAMPION randomised trial. Abraham WT, Stevenson LW, Bourge RC, et al. Wireless pulmonary artery haemodynamic monitoring in chronic heart failure: a randomised controlled trial. Abraham WT, Adamson PB, Bourge RC, et al. Spironolactone for heart failure with preserved ejection fraction. Pitt B, Pfeffer MA, Assmann SF, Boineau R, Anand IS, Claggett B, Clausell N, Desai AS, Diaz R, Fleg JL, Gordeev I, Harty B, Heitner JF, Kenwood CT, Lewis EF, O'Meara E, Probstfield JL, Shaburishvili T, Shah SJ, Solomon SD, Sweitzer NK, Yang S, McKinlay SM TOPCAT Investigators. Regional variation in patients and outcomes in the Treatment of Preserved Cardiac Function Heart Failure With an Aldosterone Antagonist (TOPCAT) trial. Pfeffer MA, Claggett B, Assmann SF, Boineau R, Anand IS, Clausell N, Desai AS, Diaz R, Fleg JL, Gordeev I, Heitner JF, Lewis EF, O'Meara E, Rouleau JL, Probstfield JL, Shaburishvili T, Shah SJ, Solomon SD, Sweitzer NK, McKinlay SM, Pitt B. End-stage heart failure with pulmonary hypertension: levosimendan to evaluate for heart transplantation alone versus combined heart-lung transplantation.Transplantation. Schulze-Neick I, Luther YC, Ewert P, Lehmkuhl HB, Hetzer R and Lange PE. An expert consensus meeting report of the Heart Failure Association of the European Society of Cardiology. Clinical practice update on heart failure 2019: pharmacotherapy, procedures, devices and patient management. Seferovic PM, Ponikowski P, Anker SD, Bauersachs J, Chioncel O, Cleland JGF, de Boer RA, Drexel H, Ben Gal T, Hill L, Jaarsma T, Jankowska EA, Anker MS, Lainscak M, Lewis BS, McDonagh T, Metra M, Milicic D, Mullens W, Piepoli MF, Rosano G, Ruschitzka F, Volterrani M, Voors AA, Filippatos G, Coats AJS. Patients were discharged from hospital within 72 hours of the procedure, and there were no complications.136. A total of 20 pulmonary veins were treated and complete acute electrical isolation was achieved in all cases (100%). These cases represent initial experience with the technique in Spain. 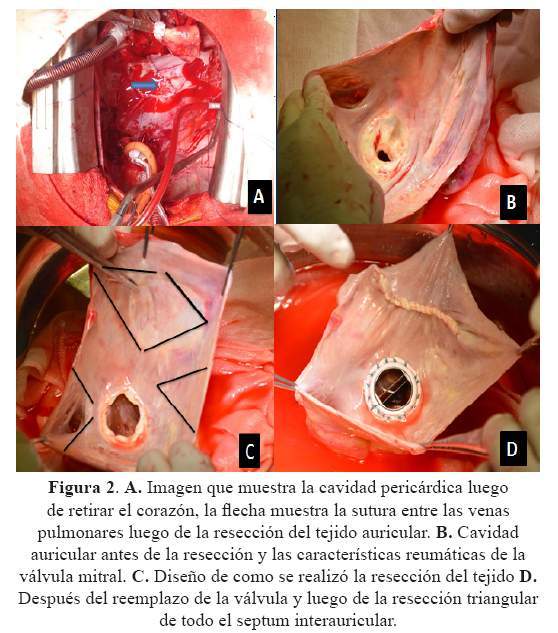
We report on immediate outcomes in the first five patients who underwent treatment. The type of lesion produced by balloon cryoablation is such that the tissue architecture is preserved and thrombus formation and the risk of pulmonary vein stenosis are reduced. En conclusión, la crioablación con catéter-balón de las venas pulmonares es una técnica factible, segura y eficaz para conseguir el objetivo final electrofisiológico de aislamiento agudo de ellas en pacientes con fibrilación auricular paroxística (AU)Įlectrical isolation of the pulmonary veins and disconnection of the left atrial musculature from their arrhythmogenic effects is the cornerstone of definitive and curative treatment in patients with symptomatic recurrent paroxysmal atrial fibrillation that is refractory to antiarrhythmic therapy. Los pacientes fueron dados de alta dentro de las primeras 72 h del procedimiento, sin complicaciones. Se trataron un total de 20 venas pulmonares, y se demostró aislamiento eléctrico agudo completo en todas (100%). Presentamos los resultados inmediatos conseguidos en los primeros 5 pacientes, que constituyen la experiencia inicial en España. La lesión producida por frío con catéter-balón preserva la arquitectura tisular, disminuye la formación de trombos y el riesgo de estenosis venosa pulmonar. 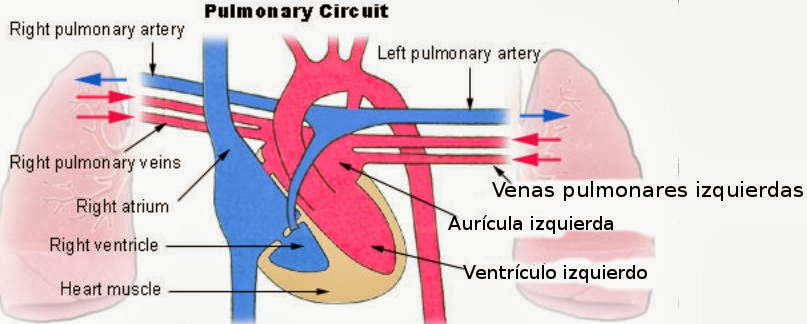
El aislamiento de las venas pulmonares y la desconexión del músculo auricular izquierdo de la actividad arritmogénica de éstas son la piedra angular del tratamiento definitivo y curativo en pacientes con fibrilación auricular paroxística recurrente y sintomática refractaria a tratamiento antiarrítmico. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
